Intra uterine Insemination (IUI) is a type of artificial insemination in which actively motile sperms are injected directly into the uterine cavity near the time of ovulation. This procedure can be performed either with partner’s sperms or with sperms from a donor. It is considered the first-line treatment for unexplained infertility, mild endometriosis, or mild male factor infertility. IUI may increase the chances of conception of the couple if the patient selection is done correctly.
Often couples undergoing an IUI cycle need support and counselling because of the emotional stress they are going through.
Couples who decide to opt for fertility treatments, tend to have a plethora of questions and often seek some guidance. Common Questions that they tend to ask are
- What will the entire process be like?
- Will the treatment or any step involved in it have any side effects or risks?
- Is the decision for going for IUI the right one?
- What is the success rate of the procedure?
- How many times will I have to opt for it?
- What are the precautions or care we need to take while the procedure is going on and even after the procedure is done?
- What are the finances involved?
And many more. ………
During this time a proper counselling from the treating doctor and a fertility counsellor can help put the couple at ease and alleviate most of their concerns.
Intrauterine Insemination (IUI) Treatment varies for every couple and involves a basic few steps before the artificial insemination process takes place. Summarized in the algorithm below (Algorithm 1)

Algorithm 1: Steps before the IUI process

Figure 1: A typical Ovarian stimulation before an IUI cycle
After a thorough history taking and evaluation when an IUI treatment cycle is advised the treatment cycle is started on day 2/3 of the menstrual cycle. Ovarian stimulation is done with the help of either oral ovulogens or injectable gonadotropins in the decided dose.Regular transvaginal ultrasounds are done on day 6, day 9 and day 11 of the menstrual period to monitor the growth of the follicles, once the lead follicles reaches a desired size of 18 to 20 mm a trigger injection is given and an IUI is done 36 to 48 hour later (Figure 1).The follicle ruptures around 36 hours after the trigger injection, and the egg once the follicle ruptures can survive for 24 hours. The IUI can be done 48 hours after the trigger injection because the process of capacitation is done in the lab. During the procedure, the male partner will be asked to provide a semen sample about an hour or two before being scheduled for insemination. This is done by masturbating into a sterile container at the doctor’s office or at home. The semen is “washed” to separate the sperm from the seminal fluid. This must be done before the sperm can be injected into the uterus because the seminal fluid contains substances that can irritate your uterus. The sample once processed should be inseminated within an hour of preparation.

Algorithm 2: What to expect on the day of the IUI
How doing an IUI may increase chances of getting pregnant ?
It reduces the effect of factors such as,
- Vaginal acidity
- Cervical mucus hostility
- Deposit motile morphologically normal sperms as close to the oocyte as possible, as close to the time of ovulation as possible
- Sperm wash techniques enhance fertilising capacity of the sperms
- IUI increases the number of sperms reaching the ampullo-isthmic junction
How does sperm washing before doing an IUI help?
- Getting rid of debris, abnormal sperms, dead sperms, seminal plasma
- Picking up good motile sperms
- In vitro capacitation
- Concentrates the motile sperms into small volume
- Eliminates prostaglandin form semen sample and there by does away with any contractions that may occur in the uterus due to the prostaglandin reaction
How does stimulating the ovaries for an IUI process help?
- Increasing the number of eggs available for fertilisation
- Overcoming subtle defects in ovulatory function and luteal phase
- Controlling the timing of ovulation
- We can time the insemination
- Stimulated ovaries come closer anatomically to the fimbrial end of the fallopian tubes hence facilitating egg pick up by the fallopian tube
- may affect tubal vascularity to enhance ovum pick up mechanisms
How is the process of IUI done?
The procedure is ideally carried out in a dedicated insemination room or the theatre with the sterilised instruments laid out on a trolley
- B)
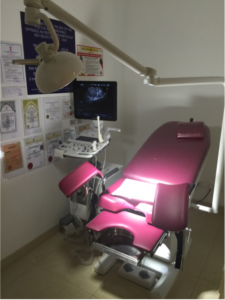

Figure 2: A) A dedicated IUI suite B) Trolley set for an IUI process
- Immediately after semen preparation (within 90 minutes of collection).
- Sample is maintained at 37°C in a test-tube warmer / held in a fist. Can be kept outside at room temperature, but not for long periods.
- Patient is asked not to void her bladder, to help correct the anteversion of the uterus
- Once the bladder is full, Lithotomy position is given
- Cervix is exposed with a bivalve (Cusco’s) speculum
- Patient identification is done by the doctor and the andrologist
- It is confirmed with the patient wether donor sample or husband sample is being used
- Insemination is done with a plastic cannula with or without ultrasound guidance
- Patient is asked to rest for 5 minutes then asked to void bladder completely
- Luteal phase support is prescribed for the next 15 days
- UPT or Bhcg is done after 15 days which tell us if the woman is pregnant or not `
Counselling sessions help to recognize various psycho-social and emotional problems faced by couples having fertility issues. The counsellors help to resolve the issue by conducting various therapies and counselling sessions.
There are various types of counselling sessions for the couples who are facing infertility issues. They include –
- Pre-treatment counselling which is a prior session before starting the fertility treatment. This counselling depends on what type of fertility treatments the couple is taking. The discussion involved in Pre-treatment counselling includes –
- Explore and discussion of any issue that might affect the treatment.
- Usually, couples might get confused about the medication which can affect the treatment. Pre-treatment counselling helps to understand the medical advice given to the couple during the treatment.
- Helps the couple to understand the rights, psychosocial, and ethical implications, responsibilities, and any legal consideration to be taken care of.
- The important details and information which the couple is not aware of are also clarified during this session.
How successful is IUI?
Couples are often curious to know about Intrauterine Insemination (IUI) treatment’s success rate and wonder if it could help them conceive and get pregnant. There are various factors which affect the IUI treatment’s success rate. There are –
- Age of a woman undergoing the IUI treatment.
- Status of the Fallopian tube
- Status of the Semen analysis
With just one IUI cycle, around 10 to 20 percent of women have the chances of getting pregnant.
The success rate of IUI treatment with one cycle with terms of age is as follows –
- 10 to 20 percent success rate for women under 35 years of age.
- 10 percent success rate for women between the age of 35 to 40 years.
- 2 to 5 percent success rate for women of the age 40 years and above.
Worldwide, the success rates for IUI is an average of about 15%. Around 80% of the pregnancies occur within the first three IUI cycles. So if the couple has not conceived in the first three cycles they need to be counselled for advanced treatment option like IVF.
Precautions
Since this is a relatively simple and safe procedure, it does not require any special precautions. Only a few minutes of rest after the procedure and then the woman can resume her routine.
The woman needs to make sure that she takes her luteal support medication as prescribed.
Possible complications
Apart from mild pain and spotting on the day of an IUI, there are no major complications. Around five to ten percent of the patients may conceive with multiple (generally twin) pregnancies. Sometimes, a patient may respond excessively to the medications and produce more eggs, putting her at risk for multiple pregnancies and a condition called Ovarian Hyper Stimulation Syndrome (OHSS). If there is a risk of this occurring, the couple is advised accordingly and the cycle may be cancelled or converted to an IVF cycle. Infection is a very rare complication.
Most of the couples need counselling to determine whether the IUI treatment is right for them or not, before moving forward with other expensive and intensive treatments like IVF. It is better to consult a doctor and a counsellor who can show the right direction. Patients who are suffering from issues like anxiety, emotional stress are offered with strategies to cope up with the problems. These can help them to carry out with the treatment smoothly. Counselling is basically a comprehensive approach that helps an individual or couples to cope up with the unusual amount of stress they go through because of infertility issues. Counsellor’s goal is to find out the strength, weakness, and support the networks, to make the patient feel better about themselves during an IUI cycle.
About The Author
Dr. Ritu Hinduja is a Senior Consultant Reproductive Medicine at NOVA IVF ( Andheri, Mumbai ).A native of Mumbai, she completed her Medicine from a town near the city of Nagpur called Wardha. She has a decade long experience in field of Fertility and IVF. In her career she has helped close to 6000 plus couples achieve their dream of parenthood. She has strikingly good success rates ,which can be vouched by parents who have conceived with her.
Dr. Ritu Hinduja is Board Certified in Obstetrics and Gynecology. While pursuing her studies she developed a keen interest in the field of Infertility which she nurtured by completing Masters in Reproductive Medicine from Homerton University, London, she has also received a Diploma in Reproductive Medicine from Keil University, Germany and a Fellowship in Infertility from Institut Marques – Spain & Assuta Hospital – Israel. Added to this she also carries a Certificate in Genetic Counselling.
Her passion and dedication resulted in her being a leading expert in all techniques of Assisted Reproduction. Dr.Ritu’s research and clinical interests include fertility preservation, poor ovarian reserve and Pre Implantation Genetic Testing.
During Her career she has received many awards and accolades for her excellent work in the field of Infertility and Reproductive Medicine a few of them are mentioned below
Awards/Prizes:
- MOGS – Shantabai Gulabchand Travelling Fellowship award
- MOGS – C G Saraiya Travelling Fellowship award
- MOGS – Banuben Nanavati Travelling fellowship award
- MOGS – Dr Pramila Bhatia Award for Best research work done
- MOGS: Dr H S Palep Award for Best Research work in Recurrent Pregnancy Loss
- FOGSI – Dr Shanti Yadav Award for Best research in Infertility
- FOGSI – Dr Kumud Tamaskar Award for Best research in Infertility
- FOGSI – Chorion award for Best research
- Wonder FOGSIAN Award
- Champion of ISAR Award
- ISAR YUVA Orator
- Recipient of the Best paper award at MOGS annual conference 2017 and 2018,
FEM conference 2017
- Central Asia Regional Conference organized by Association of Medical women in India 2010
- Best Poster award at the Annual Conference of AMOGS 2009
She is the author of numerous scientific papers and chapters and has lectured at National and International meetings and conferences. She is also an Editor of NOVAS-“Handbook of Infertility 7th Edition: Abnormalities of the Pelvis.” and Nova’s’ Text Book of Infertility. She has been a part of many decision-making panels as an expert and is a reviewer for many scientific journals.
Dr. Ritu Hinduja is a proud Elected Member of the Managing Committee Indian Society of Assisted Reproduction 2020-22 & also an elected Youth council Lead of the Mumbai Society of Obstetrician and Gynaecology (MOGS)
She loves to smile, and her patients are instantly put at ease with her warm smile. She is a Happy mom of a daughter. Her hobbies include Reading for herself and to her little one and travelling with her daughter. She strongly believes in debunking myths, breaking taboos and clearing misconceptions about Fertility & IVF and is constantly striving towards it.

